The Perfect Union: Medicine and Communications
This is not the Zambia you might know. The Zambia of tourist launches on the Zambezi River and Victoria Falls. It is a Zambia where most communication travels by foot and the sick must wait, sometimes days, for medical treatment. A Zambia desperately in need of radios to bring its doctors instantly to its patients.
In this Zambia, according to the World Health Organization, one of 16 African women dies during pregnancy and childbirth. Of the many grave statistics on health care in Africa, this is one of the most preventable. Programs focusing on maternal and child health help in many countries, however, their success is heavily dependent upon the quality and availability of medical facilities.
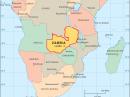
Zambia, the former British colony of Northern Rhodesia, is a large, landlocked country slightly larger than Texas, but with a population of only 9 million people. It ranks 143 out of 162 countries on the UN's Human Development Index and suffers from problems typical of most sub-Saharan African nations: HIV/AIDS (an estimated 20 percent of all adults are infected), refugees (200,000 from four neighboring countries) and economic stagnation with high debt and very little growth in its GDP. It is divided by an area of Zaire -- still referred to as the Congo -- into two sections. Luapula, the area that this project serves, is in the northwest.
The population of this province numbers over 1.5 million. In addition there are about 50,000 Congolese refuges in various nearby camps.
There is virtually no industry. The people either fish or are subsistence farmers. Although subtropical, the province is on a high plateau, ranging from 274 - 457 meters high. This altitude makes it relatively cool, with temperatures ranging from 18-26 degrees C on average during the day, according to season, and wet with up to 1.5 meters of rain per annum, falling entirely between November and April. This province is almost entirely surrounded by water and is about 100 by 400 kilometers in size. The great Lake of Tanganyika is along the Congo border to the north.
Lake Mweru beach far to the west of the Luapula River and northwest of Lake Mweru are the killing fields of the Congo (now Zaire) civil war. Refugees still cross over into Zambia at the rate estimated to be at least 200 a week even when there is no immediate fighting. Other than at Kasenga, where there are four doctors on the hospital staff, there is no infrastructure (roads, power, telephones, etc) in this vast area. Refugees migrate into Luapula Province, where they end up in the refugee camps at Kala and Mporokoso. Congolese refugees and roughly 50,000 marsh dwellers on an island in Lake Bangweulu rely on Luapula Health Services, already underfunded and understaffed. The three doctors at St Paul's Hospital on Lake Mweru, for example, estimate a true catchment area population in excess of 1 million, which is the official total population of the entire province. The Northern Area has the problem of great distances with few or no roads and nearly non-existent communications resulting from a lack of dependable power.
Due to this lack of communication and transport, the hospital receives many referral patients in bad condition. Most of these come from the northern part of Nchelenge, Chiengi and Kaputa Districts, where there are no roads, not even tarmac, few trails and little public transportation. Although the hospital has an ambulance, it cannot be used dependably because of this lack of passable roads and lack of communications with the hospital doctors.
St Paul's Hospital
St Paul's Hospital is the only hospital in Nchelenge District. This district is isolated in the extreme Northern part of Luapula Province, 450 km from Lusaka, the capital, and 250 km north of Mansa, the provisional capital.
Health services are provided by 11 Rural Health Centers (RHC) and St Paul's Hospital. The hospital serves patients from Chiebngi and Kaputa Districts, since those do not have their own hospital, and patients from the Uganda refugee camps just across the border. Nurses and/or aides -- no doctors -- staff the RHCs.
Three Major Emphases
Complicated general and, in particular, maternal patients are referred for further management to St Paul's Hospital by RHC staff or Trained Traditional Birth Attendants (known locally as TTBAs). These referrals can be delayed by a lack of communication for hours or days and might not happen at all. Most referrals are urgent and maternal and perinatal morbidity and mortality can be significantly reduced if emergency calls and consultation can be done by radio instead of by staff members who often have to walk both ways to the hospital to even gain permission to bring a patient in for treatment. This can involve a round-trip of a few kilometers to as many as 230 km (130 mi approx) -- taking several hours or even days. If the patient is accepted for treatment, he/she too must be transported by stretcher carried by two staff members walking to the hospital. It is clear that many seriously ill patients cannot physically withstand the time loss and the rigors of such a trip -- and morbidity is unnecessarily high as a result.
Until now there has been no reliable and fast way to communicate between the district health officer, the district pharmacist or personnel officer and the RNCs. This inhibited the timely offering and supply of drugs, vaccines, food for patients and other requirements to run the centers efficiently. Health center staff had to walk to Mchelenge or Chiengi to arrange for these necessities, leaving some centers without trained staff for hours or even days.
PROJECT DETAIL
The project consisted of installation of new radio equipment and solar panels to those RHCs that do not have power and communications. Also included were upgrades to the few radios already in use in the hospital, the two district health offices and the 15 Rural Health Centers. Due to either a total lack of or an erratic supply of electricity, all radios are powered with solar panels. This system makes it possible for RHC staff to consult with the doctor in the hospital -- a "luxury" not previously possible. The radios are also used to report all notifiable diseases to the District Health Officer upon diagnosis. The DHO can now communicate to the centers when a vehicle is traveling in their direction making more efficient use of the little transportation that might be available.
An important side benefit results since the solar panels are configured to provide additional power for small refrigeration units (also provided), making it possible, for the very first time, for the RHCs to store and use medications requiring refrigeration.
The radio system consists of twelve 100 W Kenwood TK-80 HF transceivers, power supplies, antennas, lightning protection, solar panels and licensing fees for one year. The project also provides training and support in the use of the equipment.
This system has been installed, tested and staff members have been trained in its use by Suntech Appropriate Technology, Ltd, a well-known and experienced communications company.
The total cost of this communications system was just over $30,000 US and was funded by a partnership between MediShare International, the Rotary Clubs of Palo Alto and Los Altos, California and Rotary International. The balance of the project, consisting of the provision of carefully selected medical equipment, instruments, supplies and drugs, was provided and funded by the Bush Hospital Foundation, on the Island of Jersey, United Kingdom. Direct Relief International, of Santa Barbara, California, provided all the equipment and material.
The information and data for this report was provided by Dr Mike Marks, Medical Director, Bush Hospital Foundation; Dr Van de Ven, Medical Officer, St Paul's Mission Hospital; Mr H. Zulu, Manager Administration, Nchelenge District Health Office; Ms Gerda Smulders, Suntech Technology, Ltd, Zambia; Ms Kathy Poma, Direct Relief International of Santa Barbara, California; Mr Joseph Chitalo, and Mr Chiman Patel, Mansa, Zambia, Rotary Club.
Photos downloaded from www.medishare.org
Robert C. Smithwick, W6CS, has been licensed for 67 years, first as W9KTL, then W7NOH and W6JZU before his current call. Smitty, as he is called, is an avid DXer having worked 350 countries. He is a veteran of WW2, having served as a dental officer in the US Navy aboard a troop transport-auxiliary hospital ship in the Pacific theater. Outside of his profession as a pediatric dentist, his principal interests have been ham radio and public education.
Over the years, he has been elected and served on two boards of trustees: One, a large multi-campus, public high school district and the second, as the Founding President of the Board of Trustees of the Foothill-DeAnza Community College District in Silicon Valley. Smitty has been told that his 46 years of continuous service is the record for the most years served in an elective office.
Smitty is currently Director Emeritus, MediShare International the creation, implementation and continuing success of which has been one of his most satisfying experiences. Smitty has a son, Michael, AA6XI, and can be reached at 25215 La Loma Dr, Los Altos Hills, CA 94022, or by e-mail at: rsmithwick@neopolitans.net
Robert C. Smithwick, W6CS
Back